“We don’t need another lesson that ends when the bell rings. We need constant, urgent training that goes beyond the classroom, right into our homes. My little sister got sick because my parents didn’t know the net had a hole. Malaria took our savings, our sleep, and almost took her. Don’t just teach me to spot the danger—train my whole family so they can save us next time. Ignorance is not a choice; it’s a lethal gap. We need the knowledge now, and we need it to stick, forever.”
A Young Girl at Ogul Primary School Takes In the Pain During Malaria Test, She Fortunately Tested Negative to Malaria.
The words of 17-year-old Daniel Ojok echo with a sense of urgency that demands our attention: “Ignorance is not a choice; it’s a lethal gap.” His plea—for training that reaches past the school class rooms and into the heart of every home—is a stark indictment of the silent epidemic that continues to ravage the region of Northern Uganda: malaria.
The recent malaria treatment and prevention training session at Ogul Primary School was led by Dr. Patricia Aciro, a health worker at Angaya Health Center 3, Unearthing a disturbing reality: Of 100 pupils tested, a staggering 54% were positive for malaria. This statistic is more than a number; it represents 54 families whose savings, sleep, and very future is under siege. It underscores precisely why the standard, infrequent health talk is failing, and why a fundamental shift to constant, comprehensive, School and family-centered training is crucial.
Pupils of Ogul Lines Up to be Tested and Checked for Malaria after a Training on Prevention and Best Practices against Malaria.
The devastating impact of this knowledge gap is acutely felt through the voice and testimony of Daniel. His family’s painful experience—losing savings and sleep because his parents “didn’t know the net had a hole”—underscores the cruel reality that a single lapse in knowledge can be catastrophic in highly endemic regions like the North of Uganda. We must heed his powerful call for training that reaches the entire family.
As Dr. Aciro asserted, “An educated child is a shield, but a trained parent is the fortress. Continuous malaria prevention knowledge must flow to the whole community to truly break the cycle of disease.” The goal isn’t just to educate the pupil; it’s to activate the most critical line of defense—the pupils, parents and the whole community—transforming a fragile lesson learned in a classroom into a resilient, practical instinct within the home and entire society.
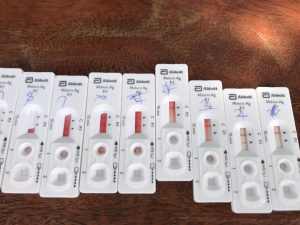
Test Results Processing to Determine the Health Status of the Pupils at Ogul Primary School.
Malaria doesn’t take a holiday or even a leave from duty, and neither can our prevention education. The training must be constant, not a one-time event, reaching every segment: young, old, school, and home. The necessity for this shift is driven by the region’s intense endemicity and a persistent knowledge-to-practice gap.
In Northern Uganda, where malaria remains the leading cause of morbidity and mortality, high infection rates translate directly into missed school days, reduced academic performance, and chronic financial strain—perpetuating cycles of poverty. Furthermore, training must be precise: it must move beyond simply telling people to use a net. It must explicitly address the deadly misuse of tools and provide practical, repetitive instruction on environmental control.
The community must recognize that draining stagnant water and proper disposal of plastics does not just deter the Anopheles mosquito, but also shields them from diseases like elephantiasis and Dengue Fever, reinforcing that prevention is a vital, and holistic defense mechanism.
Dr Patricia Making Efforts to Explain Prevention Measures to Pupils During Malaria Prevention Training in Ogul Primary School.
To achieve this instinctive defense, training must become constant and comprehensive. Institutions, such as Ogul Primary school, should be viewed as a crucial starting point, not the finish line. The health message must be channeled outwards, utilizing the energy of the learners, but supported by continuous, adult-focused education. Health workers must dedicate themselves to recurring community outreach sessions that are tailored to the realities of local life, focusing on practical skills like net repair and the early identification of severe symptoms.
When training is continuous, the message doesn’t fade, and the proper use of preventative measures shifts from a burdensome chore to an automatic, life-preserving habit.
A Young Girl Curiously Looks at other Results as Her Blood is Drawn to Test.
We must move past the one-off health talk. The 54% infection rate among the pupils of Ogul Primary School is a crisis demanding an immediate and sustained response. By committing to making malaria prevention an ingrained instinct—a defense mechanism so deeply embedded it is never forgotten—we empower every parent, every child, and every community member in Northern Uganda. Let Daniel’s powerful account, 17-year-old voice be the catalyst that transforms our passive awareness into an active, lifelong commitment, finally breaking the devastating cycle of disease and building a healthier future.
Posted By OKWIR JOSEPH JOHNS
Posted Oct 20th, 2025






1 Comment
Iain Guest
November 12, 2025
Excellent blog, Joe. You really capture the human cost of malaria, but also the inspiring work being done by health workers. I’m so impressed that GDPU is doing this great work!