This week, we have completed GDPU’s sixth malaria prevention training at Tochi Primary School. Such training is essential, especially in an area such as Northern Uganda which has amongst the highest malaria prevalence in the world.
GDPU helps its partner schools to make their own personal link with local health clinics. This ensures the longevity of the relationship between schools and clinics so they can work together again, whether on malaria training or other public health issues.
The process begins with a phone call from GDPU to the headteacher of the school introducing the idea of malaria prevention training. Most, just like Sister Mary Grace Latim at Tochi, are on board with us delivering this training.
This session at Tochi Primary School was meant to be delivered two weeks prior, however, this would have fallen in the first/second week of term. In these initial weeks, most parents don’t send their children to school as they believe the teachers will not be there so it’s a ‘waste of time’ to send them. In most schools this is not true, however Sister Mary was eager to ensure as many children benefited from this session as possible and so we delayed it.
Even still, it was disappointing to see some children running home when Sister Mary announced the training was taking place. When talking to the children who were present, she stressed the importance of this teaching, and thanked all those who stayed. However, she too was disappointed to not see the whole school present for such an important session.
A nurse and a doctor from the local health clinic led the session. The children were very excited to see the doctor – I gather he is something of a local celebrity as the doctor for the village!
Susan, the nurse, discussed with the children the causes of malaria, signs and symptoms, what to do when you first experience symptoms, and how malaria is curable but you can contract it time after time if you’re bitten again. She stressed the importance of preventing malaria, rather than curing it, and the way to do this was by sleeping under mosquito nets, using repellent oil, draining any stagnant water away and slashing bushes in the compound to minimise their breeding grounds.
The children were all very knowledgeable on this topic, even naming the specific mosquito that carries malaria (with the best known being anopheles gambiae). It was bizarre to see children this young being so technical about a communicable disease, but it’s their norm from a young age.
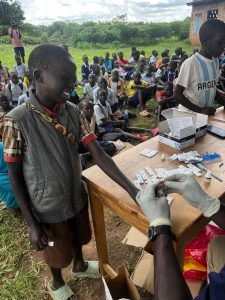
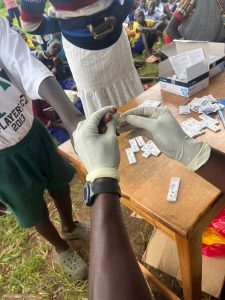
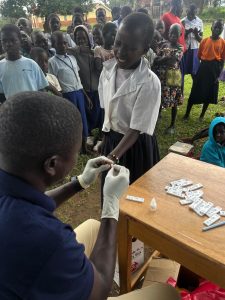
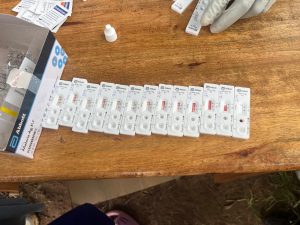
The testing begins….
Most were scared of the finger-prick….
… Others were not!
A child who particularly stood out to us all was Aloyo Princess. When we were monitoring Tochi’s toilets prior to the training session, we saw Princess leave class to sit in the sun. Joe correctly pointed out – “why would a child leave class to come and sit in the sun unless they are unwell with a fever”.
Princess was coughing and looked generally unwell. When the health workers asked for anyone who might have malaria symptoms, or anyone who wanted to get tested, to join the testing line, Princess remained seated. So, Joe went over and ensured she joined the queue.
Princess was very reluctant to get tested – I’m not sure whether that’s because she was scared of the needle prick or because in the back of her mind she knew what the result was.
After being tested, Joe had a discussion with her to understand how she was feeling about her positive result.
Princess is 14 years old and in P4. Her mother is a single parent to her and her siblings, following the death of her father when she was 8. This positive test reflected her 6th time getting malaria.
It’s alarming that she had already had malaria 5 times but did not put herself in line to be tested. This might reflect the cultural norm of viewing self medicating malaria with a simple dose of paracetamol, as reliable – whilst it might provide short term relief, it is not a cure so symptoms will return. Princess’ mother and siblings also often get sick with malaria; they have no malaria nets in their house which is likely a cause of their frequent illness.
Following the training, Princess is eager to teach her siblings about this session. She left with a deep understanding of the importance of prevention rather than treatment, and is something she seeks to educate her family on. She is also extremely keen to be given some nets for their family.
After this, I discussed with Joe how involved local health centres are in distributing nets to their local communities, and I was pleased to find out this happens frequently. So why is the malaria rate still so high? It was alarming to hear it’s purely because of greed; people take more nets than they need in case of needing more in the future. But even more alarmingly, mosquito nets are more often than not used as fishing nets and even as material for wedding dresses!
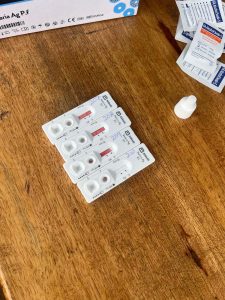
Out of the children present at the session, 66% tested positive. Without this training, it’s likely these cases would have gone undetected until their symptoms were much more severe. Sister Mary was extremely worried after being told this figure, but relieved that so many of her students would now receive treatment.
For the children who tested positive, the health clinic came prepared with anti-malaria medication. Most schools will choose for this medication to remain at school and administered to the children who tested positive each day. This prevents stockpiling of malaria medication at home, which oftentimes expires before it is even used.
The health workers also delivered some limited training on HIV/AIDs and Hepatitis B. There was less focus on these as they are slightly less prevalent, however, equally (or more) important as their impact can be much more severe. The children were equally knowledgeable on the causes, symptoms, effects and treatment for these two diseases. For these, and especially HIV/AIDs, the importance of prevention was stressed even more as there is no cure. Likewise, for Hepatitis B, prevention via vaccination is key.
Whilst discussing all these diseases is important, the result of this was a relatively brief session on malaria, despite this being the main reason we were there. This has highlighted an important change that needs to be made.
For future training, we think GDPU should put together a contract or brief for the health clinics on the topics they should deliver. The clinics, as the medical professionals, should add the substance, but we need to ensure that all children at GDPU-supported primary schools are being told similar information. For example, there should have been a greater focus on the proper use of nets, what to do if they break and where they may be able to access some nets for their family. Instead, the children were only told “nets can stop you getting malaria”.
Whilst this training and testing session was hugely beneficial to the students, it highlights malaria to be an epidemic in Uganda which requires significantly more attention that it is presently given.
Posted By Maddy Pound
Posted Oct 23rd, 2025











2 Comments
OKWIR JOSEPH JOHNS
October 24, 2025
This account powerfully illustrates the malaria crisis and the immediate, life-saving necessity of your intervention.
The 66% positive rate at Tochi Primary confirms malaria is an epidemic, not just an endemic disease. The story of Princess—a 14-year-old on her sixth bout, initially reluctant to be tested—underscores the dangerous cultural normalization of severe illness and the vital need for proactive screening. While the training is crucial, the discovery that nets are being misused for fishing and clothing highlights a critical gap: knowledge translation. Your realization that a formal contract/brief for health clinics is needed to ensure focused, actionable prevention messaging (especially on proper net use and access) is an astute and necessary refinement to maximize the impact of this essential program.
Iain Guest
October 31, 2025
Another important post about an increasingly part of the WASH program. GDPO started this last year as an experiment and your experience – like that of Aaron this summer – shows why it needs to be fully integrated into GDPO’s WASH project. First, as you say, the prevalence and threat from malaria. It’s ASTOUNDING that 66 of the students tested at Tochi tested positive. In fact, everything about this is astounding, including the fact that some of the students rushed off home instead of attending the session. Apparently the penny has still not dropped. Finally, it was so nice to see this project through the eyes of the girls. I loved how you described the anxiety but also excitement of the girls were while they waited for the tests. And it all comes alive through Princess. Getting to know her should make us all the more determined that this training is expanded and succeeds. Can’t wait to read Alex’s take on it all.